Coronavirus: Is New York City prepared to deal with thousands of cases?
Surge capacity, coordination are key
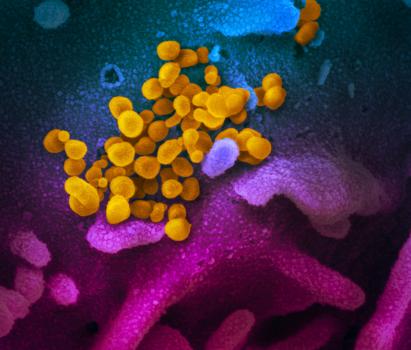
It’s only a matter of time before the novel coronavirus (COVID-19) breaks out in New York City, according to officials and the city Health Department. Is the city’s health care system ready?
That depends in part on hospitals’ “surge capacity” — the ability to handle 20-25 percent more patients than usual.
National policy calls for hospitals to accommodate surges of 500 new patients per million population in a disaster. That would amount to 4,300 additional patients across New York City. Based on population, Brooklyn would need to handle about 1,250 additional patients during a surge, and there could be two or three surges during an outbreak.

Brooklyn Boro
View MoreNew York City’s most populous borough, Brooklyn, is home to nearly 2.6 million residents. If Brooklyn were an independent city it would be the fourth largest city in the United States. While Brooklyn has become the epitome of ‘cool and hip’ in recent years, for those that were born here, raised families here and improved communities over the years, Brooklyn has never been ‘uncool’.