To avoid overdoses, some test their heroin before taking it
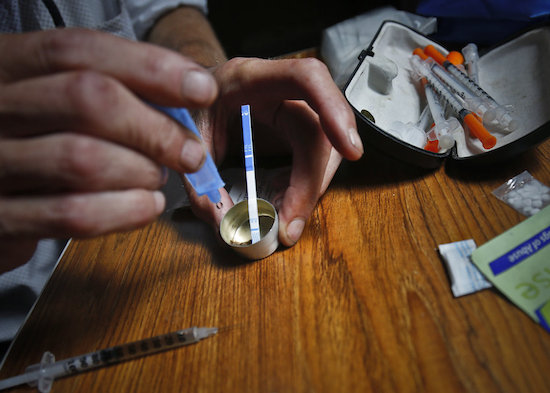
The newest tool in the fight against opioid overdoses is an inexpensive test strip that can help heroin users detect a potentially deadly contaminant in their drugs.
Sales of fentanyl test strips have exploded as a growing number of overdose-prevention programs hand them out to people who use illicit drugs.
Though they weren’t designed for it, the test strips can signal the presence of fentanyl in illicit drugs. Some health officials question their accuracy, but they have proven to be so popular that some programs can’t get enough to satisfy demand.

Brooklyn Boro
View MoreNew York City’s most populous borough, Brooklyn, is home to nearly 2.6 million residents. If Brooklyn were an independent city it would be the fourth largest city in the United States. While Brooklyn has become the epitome of ‘cool and hip’ in recent years, for those that were born here, raised families here and improved communities over the years, Brooklyn has never been ‘uncool’.